What Is Asthma?
Asthma is one of the most common chronic respiratory diseases worldwide, affecting children and adults across all age groups. According to global health estimates, more than 300 million people live with asthma, and its prevalence continues to rise due to urbanization, environmental pollution, and lifestyle changes. Despite significant advances in pharmacological therapies, asthma remains a major cause of morbidity, reduced quality of life, school and work absenteeism, and healthcare burden.
Asthma is not merely a condition of episodic breathlessness; it is a complex inflammatory disorder involving genetic predisposition, immune dysregulation, and environmental exposures.
Asthma is typically classified into different phenotypes, including allergic (atopic) asthma, non-allergic asthma, exercise-induced asthma, occupational asthma, and late-onset asthma. Although asthma is not curable, it is a manageable condition, and many individuals can achieve long-term symptom control with appropriate medical and lifestyle interventions.
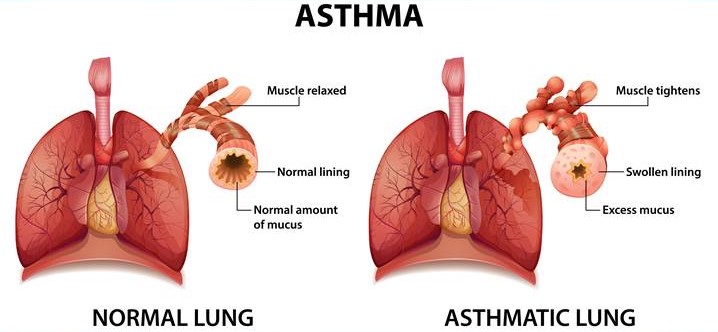
Symptoms of Asthma
Asthma symptoms vary widely in frequency and severity, both between individuals and within the same individual over time. Symptoms often worsen at night or early in the morning and may be triggered by allergens, respiratory infections, physical exertion, or environmental irritants.
Symptoms are as follows:
- Shortness of breath, especially during physical activity or at night
- Wheezing (a high-pitched whistling sound while breathing, particularly during exhalation)
- Chest tightness or a feeling of pressure in the chest
- Chronic or recurrent coughing, often worse at night or early morning
- Difficulty in breathing or rapid, shallow breathing
- Increased mucus or phlegm production in the airways
- Fatigue or reduced exercise tolerance due to impaired airflow
- Symptoms that worsen with exposure to allergens, cold air, smoke, or air pollution
Causes of Asthma
Asthma does not arise from a single cause; rather, it develops through a multifactorial interplay of genetic susceptibility, immune responses, and environmental exposures. Understanding these causes is essential for effective prevention and long-term management.
1. Genetic and Hereditary Factors
Genetic predisposition plays a significant role in asthma development. Individuals with a family history of asthma, allergic rhinitis, eczema, or other atopic conditions are at a higher risk of developing asthma. Multiple genes involved in immune regulation, airway responsiveness, and inflammatory signaling pathways have been implicated, although no single gene is solely responsible.
2. Immune System Dysregulation
Asthma is closely associated with an immune imbalance, particularly an exaggerated Th2-mediated immune response. This leads to increased production of IgE antibodies and inflammatory mediators that promote airway inflammation and hypersensitivity. Eosinophilic inflammation is a hallmark of many asthma phenotypes, contributing to tissue damage and airway narrowing.
3. Environmental and Allergen Exposure
Exposure to airborne allergens such as pollen, dust mites, mold spores, animal dander, and cockroach debris is a major trigger for allergic asthma. Environmental pollutants, including particulate matter, nitrogen dioxide, sulfur dioxide, and ozone, have been strongly linked to asthma onset and exacerbation, particularly in urban and industrial settings.
4. Respiratory Infections
Viral respiratory infections, especially during early childhood, are recognized contributors to asthma development. Respiratory syncytial virus (RSV) and rhinovirus infections may alter airway structure and immune responses, increasing long-term asthma risk.
5. Occupational and Lifestyle Factors
Certain occupations involving exposure to chemicals, fumes, or dust, such as agriculture, manufacturing, and cleaning services, are associated with occupational asthma. Lifestyle factors including smoking, secondhand smoke exposure, physical inactivity, obesity, and chronic psychological stress further exacerbate airway inflammation and asthma severity.
How Can Asthma Be Managed Naturally?
While natural management strategies should never replace prescribed medical treatment, substantial scientific evidence supports their role as complementary approaches in improving asthma control, reducing symptom burden, and enhancing overall respiratory health. Modern asthma management increasingly emphasizes an integrative approach that addresses inflammation, immune balance, environmental exposure, and lifestyle factors.
Anti-Inflammatory Nutrition and Dietary Patterns
Diet plays a crucial role in modulating systemic and airway inflammation. Diets rich in fruits, vegetables, whole grains, nuts, seeds, and healthy fats provide antioxidants, polyphenols, and micronutrients that help neutralize oxidative stress in the lungs. Vitamins C and E, carotenoids, flavonoids, and omega-3 fatty acids have demonstrated anti-inflammatory properties relevant to asthma.
Omega-3 fatty acids, particularly those derived from fatty fish, flaxseed, and walnuts, may help reduce leukotriene production and inflammatory cytokine signaling. Conversely, diets high in ultra-processed foods, refined sugars, and trans fats are associated with increased asthma prevalence and poorer symptom control.
Weight Management and Metabolic Health
Obesity is a recognized risk factor for asthma severity and reduced response to standard therapies. Excess adipose tissue promotes low-grade systemic inflammation and alters lung mechanics, worsening airflow limitation. Maintaining a healthy body weight through balanced nutrition and regular physical activity has been shown to improve asthma symptoms, lung function, and quality of life.
Physical Activity and Breathing Exercises
Regular, moderate physical activity supports cardiovascular fitness, respiratory muscle strength, and immune regulation. Although exercise can trigger bronchoconstriction in some individuals, appropriately managed physical activity improves long-term asthma control.
Breathing techniques such as diaphragmatic breathing, pursed-lip breathing, and structured methods like the Buteyko breathing technique have been studied for their potential to reduce hyperventilation, improve carbon dioxide tolerance, and decrease symptom perception. Yoga-based breathing practices have also shown promise in improving lung function and reducing stress-related asthma triggers.
Stress Reduction and Mind-Body Interventions
Psychological stress is a well-recognized trigger for asthma exacerbations, mediated through neuroimmune pathways and increased inflammatory signaling. Chronic stress can worsen airway hyperresponsiveness and reduce treatment adherence.
Mind-body interventions such as mindfulness meditation, cognitive behavioral therapy, relaxation training, and yoga may help reduce stress-induced asthma symptoms. These approaches support autonomic balance and improve patients’ ability to manage symptom flare-ups.
Environmental Control and Allergen Avoidance
Reducing exposure to known triggers is a foundational component of asthma management. Evidence supports strategies such as using allergen-impermeable bedding covers, maintaining indoor humidity below 50 percent, ensuring proper ventilation, and minimizing exposure to tobacco smoke and air pollutants.
For individuals with occupational asthma, workplace modifications and protective equipment are essential. Advances in air-quality monitoring and indoor purification technologies have further strengthened environmental control strategies in asthma care.
Evidence-Based Nutraceutical and Herbal Support
Certain nutraceuticals and plant-derived compounds have attracted scientific interest for their potential role in asthma support. Vitamin D deficiency has been consistently associated with increased asthma severity, frequent exacerbations, and reduced lung function. Adequate vitamin D status may help modulate immune responses and reduce respiratory infections.
Magnesium has bronchodilatory and anti-inflammatory properties and is sometimes used as an adjunct in acute asthma management. Herbal compounds such as ginger, turmeric (curcumin), and boswellia have demonstrated anti-inflammatory effects in experimental and clinical studies, although standardized dosing and long-term safety data remain areas of active research.
It is essential that nutraceutical use be guided by healthcare professionals to avoid interactions with conventional asthma medications.
Bottom Line
Asthma is a chronic inflammatory airway disease requiring personalized, long-term care. Alongside medical therapy, evidence-based lifestyle strategies such as anti-inflammatory nutrition, physical activity, stress reduction, and environmental control can enhance symptom control, improve quality of life, and support healthier, more active living.
- Written By: Shabina Khan (Clinical Pharmacist)
- Medically Reviewed By: Dr Sachin (MD)
